Hospitalogists,
Thanks to everyone for the outpouring of support for my ‘investigative’ piece on Done. The reception has been overwhelming, and I appreciate all of you for sharing and reading my words to expose one of the worst actors in healthcare.
Since writing the inside story on Done, countless providers have resigned from the platform, distancing themselves. The entire U.S. team is in the process of resigning, meaning the company’s operations are being run almost entirely by Chinese and Philippines-based teams.
Meanwhile, Done providers are retaining criminal defense attorneys as they’re being contacted and potentially charged with criminal charges.
Finally, I want to reiterate that one bad actor should not be enough to stop momentum in telehealth and other areas to increase access to needed care and medications across the U.S.
While scandalous stories like Done’s are very attention grabbing and sexy to write, let’s focus our attention on the teams who make clinically rigorous, rather than financially motivated, decisions.
On to this week’s news!

SPONSORED BY PEARL HEALTH
Don’t miss Pearl Health’s upcoming webinar, ACO REACH or MSSP: Which Is Right for You?, next Thursday, June 27th at 2:30pm ET.
With the CMS enrollment deadline fast approaching on August 1st, many primary care organizations and hospital systems are under pressure to evaluate the right mix of value-based care models for 2025.
Join next week’s webinar for an overview of ACO REACH and MSSP, and a deeper dive into:
- Financial, administrative, and clinical considerations and tradeoffs;
- Key questions to help you determine the right mix of VBC models for your organization; and
- How Pearl supports success in both programs with the right finances, technology, and services.
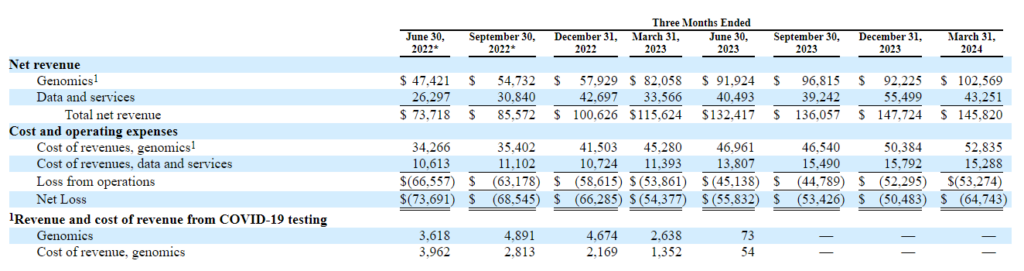
Tempus AI IPO debut is a success…initially
Tempus announced its initial public offering (IPO) of 11,100,000 shares of Class A common stock at $37.00 per share, raising proceeds of around $411 million on June 13.

While Tempus’ initial debut was successful (up 9% on day 1 and pricing at the high end of its given IPO share range), subsequent days have not been so kind. As of this writing, Tempus shares are down 26% from its initial pricing of $37/share. (Tempus S-1).
You’re Done.
Digital Health Fraud Scheme: The founder and CEO of Done Global Inc., Ruthia He, and its clinical president, David Brody, were arrested for their roles in a $100 million scheme involving the illegal distribution of Adderall and healthcare fraud. They allegedly exploited telemedicine to prescribe over 40 million pills without proper medical oversight and committed fraud by submitting false claims to Medicare, Medicaid, and private insurers. This marks the DOJ’s first criminal drug distribution prosecution involving a digital health company (Read the inside story of Done’s malpractice from me here)
Recalculated star ratings benefit Medicare Advantage Players
Medicare Recalculates Advantage Plan Ratings: Medicare is set to recalculate the quality ratings for Medicare Advantage plans to ensure more accurate assessments. The initiative comes at somewhat of a surprise, and aims to reflect true plan performance and provide better information for beneficiaries.
Join the thousands of healthcare professionals who read Hospitalogy
Subscribe to get expert analysis on healthcare M&A, strategy, finance, and markets.
No spam. Unsubscribe any time.
MA players will receive a reprieve from the 2024 Medicare Advantage onslaught as CMS recalculates star ratings and certain players like SCAN, Elevance, and Humana will receive adjustments upwards in the hundreds of millions of dollars range. Per the WSJ article, there will be no downward adjustments based on the new calculation methodology.
- “SCAN executives estimated that a redo of the quality ratings could result in more than $1 billion in additional payments to insurers, affecting about 60 Medicare contracts covering more than a million members. Raymond James analysts estimated the current star ratings cost Humana about $150 million in bonus payments and UnitedHealth Group $70 million in bonuses.”
As a result of the new calculation, MA plans will tweak and recalculate bids for 2025.
Strategy Spotlight
Key considerations for decision makers. Notable moves, policies, and strategies.
Enhabit’s Strategic Stabilization: Enhabit is between a rock and a hard place with a board battle against activist investor group AREX Capital Management. As part of a recent investor update, Enhabit is pleading with its stockholders to vote against AREX board recommendations noting that its operating environment as a recently spun off home health & hospice agency (from Encompass) has been difficult.
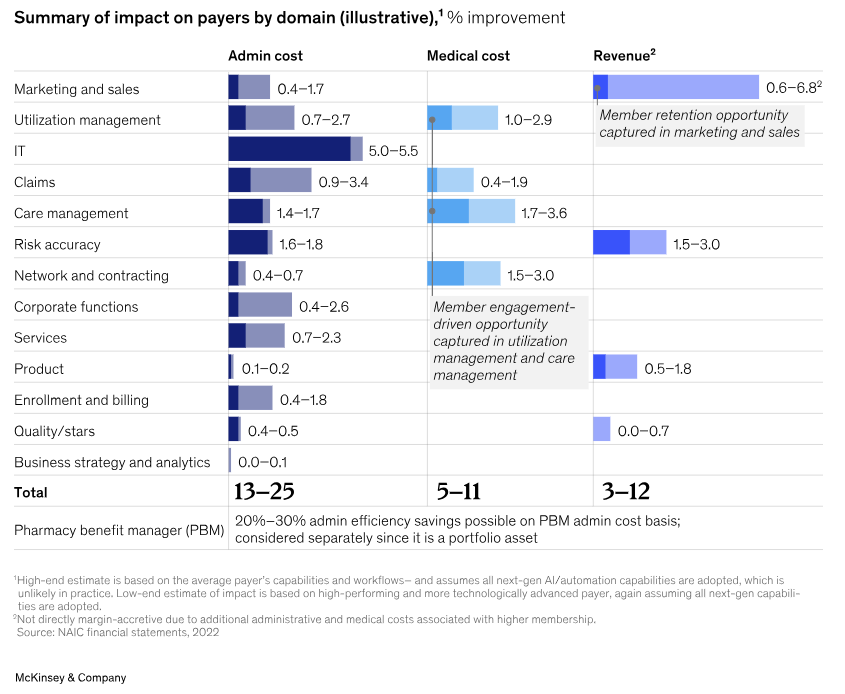
AI Opportunity for Payors: A McKinsey study finds payors can leverage AI and automation to reduce administrative costs by 13-25%, medical costs by 5-11%, and increase revenue by 3-12%.
Salesforce Expands in Healthcare: Salesforce is enhancing its presence in healthcare by introducing AI tools like Einstein Copilot: Health Actions, aimed at automating clinical summaries and improving patient data insights. The company offers solutions such as Data Cloud for Health and MuleSoft Direct for Health Cloud to integrate data from electronic health records and claims systems.
Private Equity in Healthcare: This was an interesting look from Cardiovascular Business into certain stakeholder commentary on the FTC’s workshop on private equity in healthcare. Concerns include potential negative impacts on patient care, competition, and clinician autonomy, with some stakeholders highlighting benefits like increased capital and innovation. Notable voices like Elizabeth Warren (go figure) and multiple state attorneys general brought up the risks of market dominance, higher prices, and reduced care quality, advocating for enhanced regulatory oversight and transparency to protect patient interests.
SCOTUS Reviews DSH Payments Case: The Supreme Court will review a case challenging the HHS formula for calculating Disproportionate Share Hospital (DSH) payments, affecting over 200 hospitals. These hospitals argue that the current method undercounts care provided to Supplemental Security Income (SSI) patients, costing them over a billion dollars annually – potentially altering funding for programs like 340B.
Humana’s Value-Based Care Success: Humana published findings this week that its VBC model has led to a 5% reduction in unnecessary hospital admissions among Medicare Advantage members with chronic kidney disease. Since 2019, this approach has lowered the medical expense ratio for these patients by over 12%. Humana collaborates with various partners, including Evergreen Nephrology and DaVita, to manage care for more than 77,000 kidney patients.
SCOTUS Ruling on Medical Debt: The Supreme Court has upheld the Consumer Financial Protection Bureau’s (CFPB) funding through the Federal Reserve, rejecting a challenge that could have disrupted its operations. This decision allows the CFPB to continue targeting aggressive medical debt collection practices, protecting over 100 million patients from potential financial harm. Proposed regulations include barring medical debt reporting to creditors and employers, which would safeguard consumers’ creditworthiness and reduce the financial burden on those with healthcare debt.
FDA Expands RSV Vaccine Eligibility: The FDA has expanded the approval of GSK’s respiratory syncytial virus (RSV) vaccine, Arexvy, to include adults aged 50 to 59 who are at risk of severe illness.
Cone Health’s $100M Turnaround: A good look from Beckers inside Cone Health’s $100M financial turnaround including reduction of contract labor (probably the biggest lever here), hiring international nurses, and outsourcing certain staff functions.
Rise in Cancer Incidences: A cohort study analyzing cancer incidence trends across successive social generations in the U.S. found significant increases in cancer rates among Generation X (born 1965-1980) compared to previous generations. While lung and cervical cancers have decreased, other cancer types have seen notable rises.
Supreme Court on Mailed Abortion Pills: The Supreme Court unanimously upheld the legality of mailing abortion pills, rejecting challenges that sought to limit access to mifepristone, a commonly used medication for terminating pregnancies.
Michigan Insurer Drops Weight-Loss Drugs: Michigan’s Blue Cross Blue Shield announced it will stop covering weight-loss drugs, including popular medications like Wegovy and Saxenda, starting in 2024. It’ll affect around 10,000 people and maybe we’re starting to see the shiny GLP-1 object lose its luster a bit also given this BCBS report on real-world trends in GLP-1 treatment persistence describing 6 in 10 adults discontinue GLP-1s before seeing any clinical benefit.
Notable TEAM Model Comments: The proposed Transforming Episode Accountability Model (TEAM) by CMS has sparked significant feedback. Stakeholders, including hospitals and physician groups, oppose making the model mandatory, citing concerns over increased administrative burdens and financial strain, particularly for rural and safety-net hospitals. Key suggestions include making the model voluntary, extending the transition period to financial risk, and revising benchmarks and risk adjustment methodologies to better reflect diverse care scenarios (McDermott+Consulting).
IVF Morally Acceptable: A Gallup poll reveals that 82% of Americans consider in vitro fertilization (IVF) to be morally acceptable, reflecting broad societal support for the procedure. The poll comes at a similar timeframe to some shenanigans between Senate Republicans & Democrats around a divided IVF bill.
IU Health Removes Noncompete Clauses: In a fascinating move, IU Health will eliminate noncompete clauses from contracts with primary care providers, effective December 15, 2024. This change follows state legislation banning such clauses in new provider contracts and aligns with the Federal Trade Commission’s stance against noncompete agreements. IU Health must have looked up and said “well we control most of the market anyway, wouldn’t hurt to throw the FTC a bone.”
Decent Health’s Comeback: This Fierce article was a good look at Decent Health, after a major setback in January 2023, has relaunched with a new strategy focusing on level-funded employer health plans centered around direct primary care. The approach enables Decent to offer health plans that are 40% less costly than traditional options, aiming to serve small and medium-sized companies. The company’s efforts include partnerships with One Medical and Hint Health.
Partnership Pulse
Collaborations and launches to keep a pulse on.
- WakeMed selects Bamboo Health to drive improved care coordination for patients.
- AMSURG and Palomar Health form a strategic surgery center partnership.
- Clover Health announces Counterpart Health, a new SaaS and tech-enabled services solution to bring CA technology to all Medicare Advantage payors and providers.
- Pager Health and League partner for maternity care for underserved populations.
- UltraSight and Mayo Clinic develop AI-powered algorithms for image analysis.
- Tampa General Hospital selects Palantir’s AI software to power connected care coordination, extending their long-term partnership.
- CHRISTUS Health reduces cognitive load on clinicians by 78% with Abridge.
- Verily unveils a new chronic care platform called Lightpath.
- Innovaccer expands its HXP capabilities with the launch of an AI-powered healthcare contact center.
- Clear expands its footprint in healthcare with InterSystems and Epic partnerships.
- DeepScribe collaborates with Texas Oncology to provide AI solutions for complex patient documentation.
- Alma announces generative AI-powered progress notes to reduce therapist burnout and improve client outcomes.
- Imperium Health partners with DecisionRx to deliver no-cost medication therapy optimization to Medicare beneficiaries enrolled in its Accountable Care Organizations.
- OneOncology partners with Connecticut Oncology Group.
- Tampa General Hospital deploys artificial intelligence tools to elevate patient experience.
- Headspace partners with Uwill to expand mental health offerings to students.
- Christus Health deploys Abridge’s generative AI tool for clinical documentation.
- Brightside Health expands into substance use disorder and virtual intensive outpatient treatment.
- UW Health nurses test AI tools for patient messaging.
- Clever Care Health Plan, Inc. partners with MHK to support membership growth initiatives.
- CipherHealth launches AI summaries to transform patient rounding.
- HealthTap expands access to affordable primary care to 280 million Americans by accepting insurance for all visits.
- HubSpot announces HIPAA-compliant tools in public beta.
- Nurse.com unveils next-generation talent marketplace to revolutionize healthcare hiring.
Hospitalogy Top Reads
My favorite healthcare essays from the week
MedPAC’s June report to Congress was published late last week, always chock full of good information and recommendations for policymakers to think about.
A good article from the WSJ on vertical integration in healthcare: What Happens When Your Insurer Is Also Your Doctor and Your Pharmacist
Health Affairs published a nice summary on CMS’ annual release of national expenditure projections from 2023 – 2032. In summary, total healthcare spending bumped up to $4.8T.
