Back in August, I wrote about Arbital Health as the infrastructure layer VBC desperately needs. The knife slicing through the onion that is the complexity of taking on risk. The shared rails that payors, providers, and risk-bearing orgs could finally run on together.
Arbital’s core thesis about enabling better VBC hasn’t changed. What’s changed is Arbital sharpened the knife further.
Since our last conversation about Arbital, the AI-enabled actuarial platform has been steadily deploying new products. In September and October 2025 Arbital announced its proprietary contract financials dashboard and launched Merlin AI shortly thereafter.
Today we’re diving into Merlin AI, Arbital’s Actuarial AI assistant, and the reason I’m writing about this company again. Merlin AI is the first actuarially trained, purpose-built AI platform designed specifically for contract management. And before you roll your eyes at yet another healthcare company claiming “AI” magic on a fluffy website, hear me out. This one is purpose built by actuaries, FOR actuaries and C-suite leaders at risk-bearing firms. Those are the guys and gals performing the black magic witchcraft (otherwise known as ‘math’) crucial for the foundation of managing populations and associated risk. And, as most Hospitalogists know, the market timing could not be more relevant given the current risk backdrop.

The Market Is Screaming for This
Putting this all into context is important, especially as I think we’re at a huge crossroads when it comes to risk-bearing organizations. Medicare Advantage has been the main engine for value-based care, but the large carriers have been hemorrhaging money over the past 2 years. 2026 isn’t getting much better with the infamous flat advance rate notice and ongoing v28 changes. UnitedHealth, Humana, CVS, Elevance…pick your favorite earnings call and you heard the same story: elevated MLRs, with utilization running hotter than models predicted (+10% in some instances).
At the highest level, employers are sounding the alarm around spend trend. National health spending is projected to grow 7.1% in 2025, outpacing GDP and putting even more strain on forecasts and margins. Cost trends shifted faster than internal models could reconcile.
Now, there are some interesting downstream consequences playing out right now. Optum is pulling back from VBC contracts, writing down their value. They’re tightening up their affiliate network by 20% and many carriers pulled out of MA markets across the nation. As mentioned, CMS dropped an advance rate notice (on the day of UnitedHealth’s earnings no less!) that kicked everybody in the teeth. Major payors are discontinuing risk arrangements. That seems counter to CMS’s stated goal of enrolling 100% of Traditional Medicare beneficiaries in accountable care relationships by 2030.
What’s interesting is that payors will try to offload as much risk as they can onto other risk-bearing entities willing to take the…risk. So we may see a short-term boost in sub-capitation and a revitalization of value-based care, of sorts. But the first question you need to be asking yourself before you take that risk on is…”why is this massive carrier so eager to push these contracts onto me?”
So my thesis is that value-based care, in short order, is going to separate itself between the models that work and can take risk on appropriately, using tools like Merlin AI and Arbital to provide real-time insights into what’s happening across their populations and local markets, and those that try to play the scale game without actually doing any blocking and tackling.
VBC isn’t failing because the concept is wrong. VBC is failing because we’ve been building a house on a faulty foundation. We’re asking organizations to take on financial risk without giving them the infrastructure to manage it. We’re placing an impossible burden on actuarial teams, often without the tools or resourcing they need to anticipate what’s coming next. Finance and actuarial teams are left reconstructing performance after the fact rather than being empowered with next best actions to bend the risk curve back as soon as trends arise.
And this ‘in the moment’ is the foundational crack that Arbital, and Merlin AI, fills.
Merlin AI the Black Magic Wizard Supercharged, Actuary-Trained AI Assistant
At the Hospitalogy VBC retreat, we joked that actuaries are black magic wizards. Nobody really understands what they do, everyone knows the math matters, and the handful of people who get it are worth their weight in gold. The problem is that most risk-bearing organizations (especially providers) don’t have large actuarial teams. They’re drawing from overworked analytics staff, stitching together performance metrics from multiple payors, each with different service categories and quality definitions. And, even in large payers that have actuarial teams, data is scattered. Reports from various markets, or even a single market (!!), take weeks. So by the time leadership gets a clear picture, your performance year can die to a few high cost patients.
Merlin AI changes the speed of that loop from months to minutes. But speed alone isn’t the differentiator.
Merlin AI is fine-tuned on Actuarial Data. If you dump the same claims data into ChatGPT that you put into Merlin AI, you’re going to get wildly different outputs. ChatGPT will give you some generic garbage. But Merlin AI provides actuarially grounded next-best actions with full traceability back to the logic, data, and models behind every conclusion (since I know you VBC nerds like your numbers). Every insight is deterministic, auditable, and defensible.
The platform reads and structures your contracts, extracts every financial parameter (MLR targets, PMPM thresholds, risk corridors, quality gates, shared savings splits), and aligns them with Arbital’s validated actuarial and predictive models. From there, you can ask Merlin AI nuanced questions in plain language. Here are some real-time queries users have made in the past to get actionable results:
- “What is my current PMPM and MLR by market and year?”
- “Show monthly trends for inpatient admits, ER visits, and readmissions over the past 36 months”
- “What is our PMPM for [specific state and market] Medicare?”
- “How many ER and in-patient admits did we have in 2025 for Medicare and Medicaid?”
- “Can you get me the total ER spend by member? Include visit count, line of business and market.”
- “Who are my most expensive members in Arizona?”
- “Can you give me a list of Medicare members in Arizona whose total claims exceeded $250,000 in 2025?”
- “Create a chart of disease prevalence in 2025 for Payer A and compare that to Payer B”
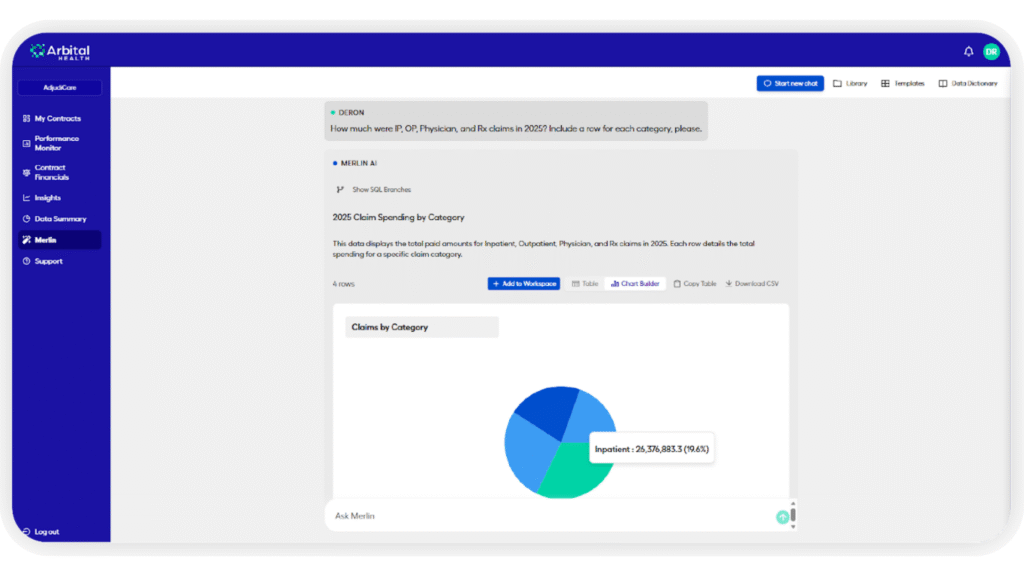
Merlin AI returns answers generated from your own data, not canned content, in tabular or visual formats your team can act on immediately.
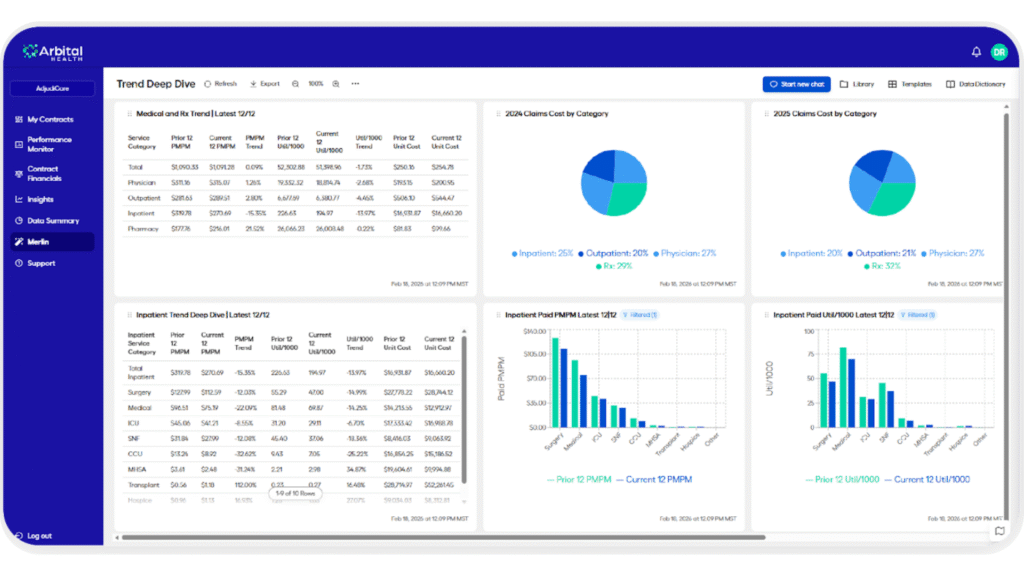
And the kicker: you can click through to see exactly why Merlin AI reached its conclusion. What model it used. What data informed the output. What logic chain it followed. This is the difference between healthcare AI and what Arbital calls Actuarial AI, a new category where the AI doesn’t just tell you what to do but shows you why, with the rigor and transparency an actuary would demand. Finance teams can report on it. Compliance can audit it. Your chief actuary can trust it.
How does this translate into better performance? In the spirit of the nerds who are reading this (I’m KIDDING guys alright), let’s talk real numbers. Arbital passed along some ROI data to me for a standard 50K member MA group. In that group, Merlin AI identifies actionable cohorts:
- Missing/suspect HCCs: Recapturing 25% of identified gaps can unlock $21M in risk-adjusted revenue
- Avoidable admissions: Engaging 50% of 2,500 flagged members and reducing 75% of avoidable admits saves $4M
- Elective surgeries: Reaching 50% of members planning elective procedures and avoiding 30% saves $2M End-of-life: Engaging 50% of 3,000 EOL members with earlier hospice transitions saves $15M
- Frequent flyers: Intervening on 33% of 500 members costing $9K+/month with a 20% cost reduction delivers a $3.5M return
These aren’t hypothetical projections. Arbital’s predictive models are embedded directly in Merlin AI, so teams can identify their highest-cost HCCs, list them out, and take action within seconds. Before Merlin AI, a chief actuary at one client could analyze one market per month after waiting on data pulls requested from another team. After go-live, the actuarial team had visibility into all markets simultaneously, spotted a pharmacy cost spike in one region, and moved to manage the trend before it blew up the contract. Care teams didn’t even need to wait for the actuarial report. They logged in and acted on live data.
For a CFO, that shift from reactive to proactive is everything. VBC contracts take years to negotiate and reach maturity. To burn an entire performance year only to discover the contract is underwater, when you could have changed protocols around certain populations months earlier, is a massive and avoidable opportunity cost.
Merlin AI’s Secret Sauce: Confirmed Not a Wand
I want to re-emphasize the point that Merlin AI is built differently.
Arbital was built on a foundation of actuarial expertise. The company made two acquisitions of actuary companies and has since built a team of 25+ extremely high-level actuaries in-house. These core team members have spent their careers living and breathing inside real risk contracts with payors and providers.
Arbital hires what they call actuarial engineers: professionals with the rare dual skill set to both understand actuarial thinking and translate that thinking into technology. These are the people training Merlin AI. The actuarial logic, rules, completion factors, IBNR methods, and settlement math aren’t bolted on as an afterthought. They’re core to the platform because the people who built it are the same people who’ve been doing this work manually for decades.
That depth of domain expertise is a key distinguishing factor separating Merlin AI, and this entirely new category of Actuarial AI that Arbital is leading. Experience and trust matter in healthcare, bar none.
Why This Matters Right Now
Merlin AI is already delivering value. Clients are logging in daily, asking ad-hoc questions in the flow of business, and getting immediate, decision-ready answers from their own data. The platform is evolving fast, with new modules and capabilities shipping daily (Arbital also closed a $31M Series B led by Valtruis in mid 2025 to fuel deeper payor capabilities and portfolio scale).
Their roadmap points toward even more sophisticated workflows: asking Merlin AI to prioritize a member list for risk of future inpatient or ER admissions and recommending the shortest path to impact.
I know every healthcare company has an AI story right now, but most of them are vaporware dressed in a nice pitch deck. Arbital’s story is different because, plain and simple, their foundation is different. Twenty-five actuaries who’ve lived inside risk contracts. A platform that digitizes contract logic and measures performance continuously while risk deals are in-flight. Benchmarking that matches members to digital twins in near-real time. And now an AI layer that doesn’t just surface insights but shows its work, the way an actuary would, so leadership can actually trust and act on what it sees.
Value-based care does not have to be this hard. Arbital is proving that thesis one contract at a time.
Get in touch with the Arbital Health team here if you’re a risk-bearing org looking to stop flying blind. In my humble opinion, this is a must-take meeting.
Join my Hospitalogy Membership! If you’re a VP or Director working in strategy or corporate development at a hospital, health system or provider organization, you will get a lot of value out of my community as I purpose-build the content, fireside chats, and conversations for this group. Apply Here.
